PLATELETS AND TISSUE REMODELING
The field of medicine is advancing rapidly towards the development of less invasive procedures and the idea of “biological solutions to biological and medical problems” is gaining ground. In the last few years, one important development of such biological preparation is platelet-rich therapy (PRT). The application of PRT has revolutionized the field of regenerative medicine largely due to the repair capacities of the growth factors and proteins secreted by platelets.
Platelets are well known for its role in blood clotting. Blood platelets are produced in large numbers from their parent cell, the megakaryocyte, which matures in the bone marrow. Despite its tiny size (1 – 3 μm), having no nucleus and living a short life span of only 7 to 10 days, platelets are packed with a large number of storage organelles. Each platelet resembles a large manufacturing plant that produces growth factors, chemokines, cytokines, proteins and neurotransmitter. Figure 1 depicts a summary of the amazingly rich storage of bioactive factors in a platelet.
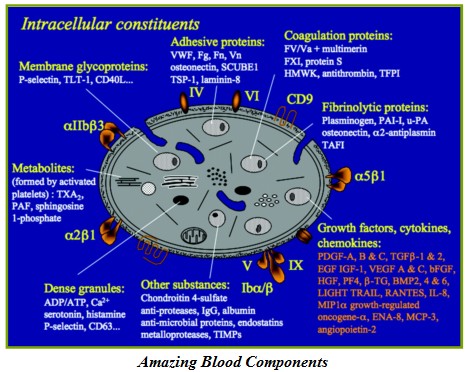
Although the role of all the growth factors involved in tissue regeneration is only partially elucidated, the potential benefits of many of them have been demonstrated. For example, platelet-derived growth factor (PDGF) is a powerful stimulator for connective tissue cells, transforming growth factor-β (TGF-β) activates bone stem cells to proliferate, insulin-like growth factor (IGF-I) promotes maturation of bone cells, and vascular endothelial growth factor (VEGF) induces blood vessel repair and formation. Platelets also secrete a neurotransmitter, serotonin, which mediates liver regeneration as one of the many benefits seen.
In light of these discoveries, there have been great emergences of the clinical use of autologous PRT in many different fields, including orthopedics, sport medicine, dentistry, cosmetic and periodontal medicine, plastic and maxillofacial surgery.
In our clinic, we extract venous blood to obtain platelets which are such an easily accessible reservoir of growth factors and bioactive protein. After the blood is separated by centrifugation, the platelets will be activated to release its storage into the plasma. This activated platelet rich product will then be reinjected either intravenously and or locally into the problematic area. The efficiency of this process lies in the delivery of a wide range of growth factors and proteins, performing the physiological reparative and regenerative processes.
If we liken the human body to an automobile, the stem cell therapy would be an overhaul of the engine, whereas the platelet rich therapy would be an oil change. If our vehicle needs regular servicing, our body certainly demands at least the same care!
